In a world saturated with fleeting beauty trends and quick-fix solutions, a new paradigm of skincare is emerging – one that looks beyond the surface to cultivate lasting skin health from within. This is the realm of the holistic skin coach, a professional who blends the art of coaching with the science of dermatology to…
Category: Dermatology Archives
Welcome back to “Skincare Deep Dive,” our brand new series on the acne podcast where we explore the science and soul of skincare. Today, we’re diving into a topic that affects millions: acne. But we’re not just talking about the usual creams and cleansers. We’re asking a bigger question: Is the future of acne treatment…
Hello and welcome to Skin Deep Dive, a brand new podcast series on The Acne Podcast by me Dr.TWL, and today we’re tackling a topic that floods the aisles and our social media feeds: acne ingredients. If you’ve ever stood bewildered in front of a shelf packed with spot treatments, cleansers, and serums, all promising…
In this workshop, we will be covering the following The following is a lip care routine I designed, as part of my work on developing lip cosmeceuticals. FAQ How is skin on the lips different from the rest of facial skin? The lips are a delicate part of your facial skin that is distinct because…
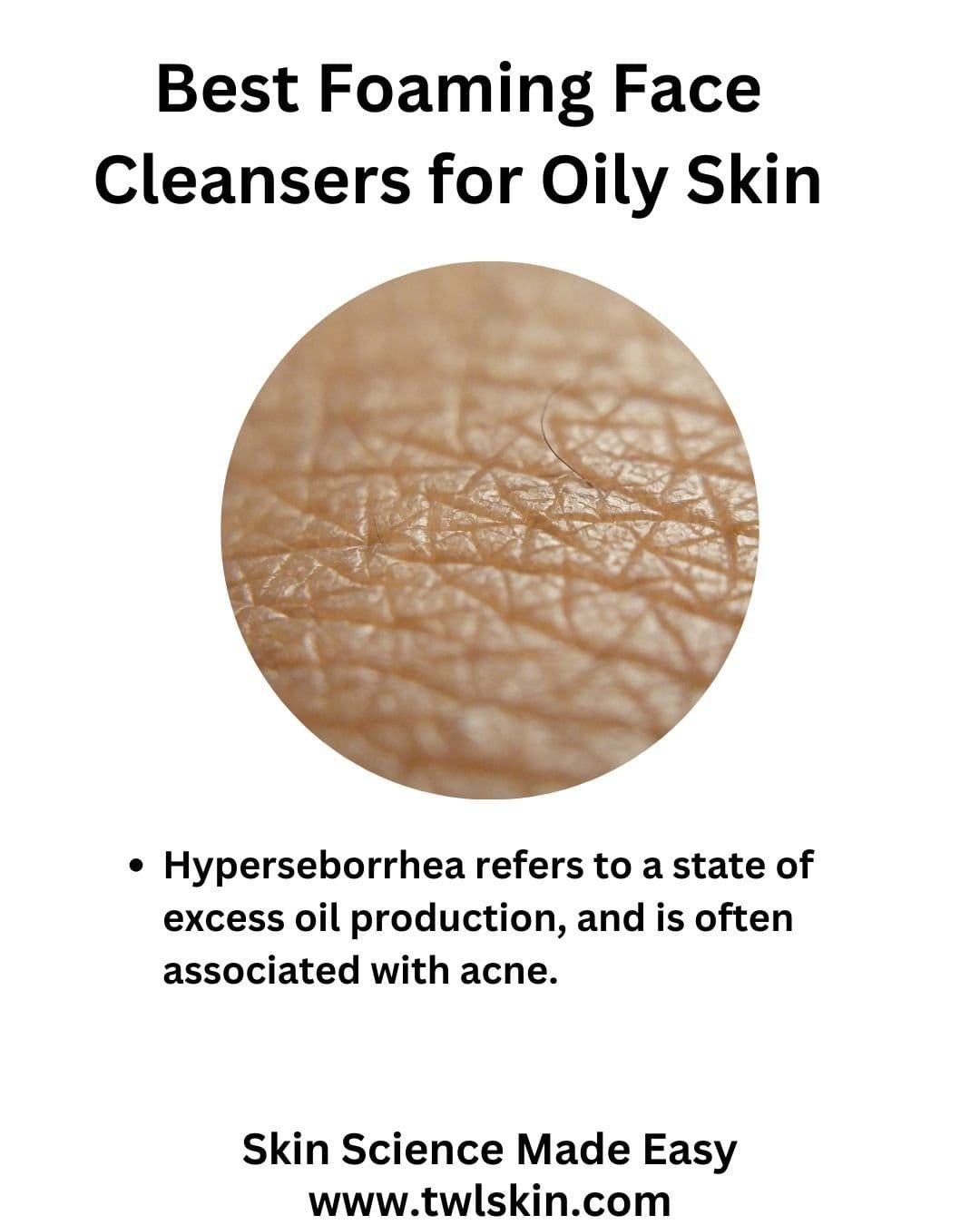
Did you know that the best foam cleanser for oily skin is one that actually shouldn’t dry out your skin? In this week’s tutorial I’m going to spill the beans on how to harmonize oily skin from the outside in. Download your complimentary worksheet here. Sign up for our free Skincare Blueprint: Glow Up From Within newsletter to receive our…
The Skincare Decoded book is a 3-in-1 special edition, comprising the Skincare Bible and the workbook in a single reference textbook, plus a full suite of online materials including digital slide show access, and expert workshops on the skin barrier. For a limited time only, get the best-selling Skincare and Medifacial Expert course by Skin…
You may already be aware of the importance of skin barrier function—how it can affect the condition of the skin, but how exactly? Skin hydration and the stratum corneum barrier have been active areas of dermatologic research for a good decade. Alongside these developments, consumers are beginning to find their interest piqued about the subject, largely…
If you are wondering how to treat pigmentation on sensitive skin, this tutorial is for you. Part 2 of the Skincare Formulation Series by Skin Masters Academy brings you the delicate art of treating pigmentation while balancing the needs of sensitive skin. This series is written for advanced skincare practitioners who are interested in the…
Skincare courses by Dr.TWL Skin Masters Academy offer an in-depth study into the science of skincare and practice of basic dermatology taught by board-certified dermatologist Dr Teo Wan Lin. As an international beauty KOL, Dr Teo has collaborated with leading skincare brands such as Eucerin, Skinceuticals, L’Oreal Paris to name a few on her podcast…
In a rapidly evolving beauty landscape, the modern consumer pursues not just visible results, but scientific authenticity and safety from every product. The concept of a dermatologist formulated skincare manufacturer has emerged as the gold standard in precision skincare—where clinical expertise leads formulation science, device innovation, and even the packaging used for daily rituals. Dermatologist…